What is a ganglion?
A ganglion is the most common lump found in the hand and they are benign lesions. A ganglion is best thought of as a sac (or cyst) arising from an adjacent joint capsule or tendon sheath. The cyst is filled with a thick jelly-like substance. A ganglion can arise from several areas in the hand and wrist, but the most common sites for presentation are:
- back of the wrist (figures 1 & 2)
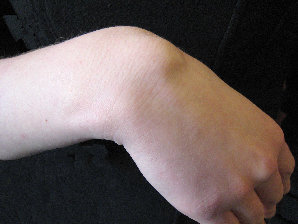
Figure 1: typical appearance of s ganglion on the dorsal wrist.
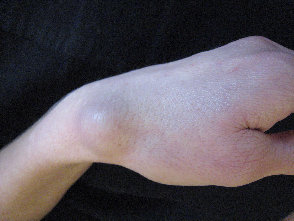
Figure 2: a large ganglion on the back of the wrist.
- base of the thumb on the palmar side of the wrist (figure 3)

Figure 3: a lage ganglion on the palmar surface of the wrist.
- end finger joint (called a mucoid cyst - figure 4)
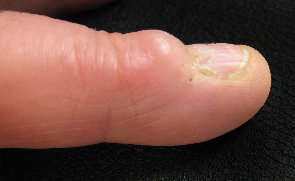
Figure 4: a large mucoid cyst at the end of the finger causing grooving of the fingernail
- base of the finger in the palm (called a flexor sheath or 'pearl' ganglion)
Despite being common ganglions, the exact cause remains uncertain. The most popular theory is that they form as part of a degenerative process of the tissue that is responsible for producing the synovial fluid which normally lubricates the joint of tendon sheath. The ganglion develops as this fluid accumulates outside the joint or tendon sheath in a sac or cyst. In mucoid cysts the ganglion develops as a consequence of underlying joint osteoarthritis and there may be pain on joint movement.
Symptoms and signs:
Ganglions usually present as a lump in one of the typical areas described above, which may be cosmetically unsightly. These lumps often do not cause any symptoms but they can be uncomfortable, painful or locally tender. They classically fluctuate in size, becoming bigger and smaller. Ganglions at the end of the finger can cause deformities of the fingernail and sometimes they spontaneously discharge releasing a clear jelly from the nail fold. When this happens a secondary infection may develop. Patients with flexor sheath (pearl) ganglions may experience discomfort in the palm when objects are gripped in the hand.
Your doctor will usually diagnose a ganglion without additional investigations. The lumps are typically hard to touch and often feel like a bony lump. They occur usually at the classical anatomical areas and if a torch is pushed up against the lump it permits the light passing through the substance (transilluminates). X-rays may be helpful in ganglions affecting the finger as there is often osteoarthritis present.
Treatment:
In some patients the ganglion can spontaneously disappear and no treatment is necessary. Other patients may be reassured that the lump is benign and may choose not to have any treatment. For those for whom the ganglion is either unsightly or painful, treatment is available.
Non-surgical
It is possible to insert a needle into the ganglion and remove the jelly like contents (aspirate). This is a minor procedure, it confirms the diagnosis if there is any doubt and it removes the lump. The main problem with this treatment is that the lump is likely to come back in as many as 80% of cases.
Surgical
Surgery is the most reliable method of removing the ganglion. The surgery is performed on an outpatient basis and the ganglions on the finger are removed using local anaesthesia. Ganglions on the wrist are usually removed either using general or regional anaesthesia (the local anaesthetic is injected into the shoulder region which temporarily makes the arm numb). The surgery is relatively minor taking 15-20 minutes. Following surgery, a light dressing is applied to protect the wound but early active movement of the fingers and thumb is encouraged. The dressing will remain for up to two weeks after the operation and it is recommended that the hand is kept dry during this period.
There are several recognised complications following surgery:
- wound infection (approximately 1%)
- there will be a visible scar which may be tender for a period
- stiffness of the fingers or wrist (uncommon)
- recurrence of the ganglion (up to 20%)
Most people do not have any problems after their surgery and the lump is permanently removed. One of the biggest problems is that the ganglion can return, which does not necessarily mean that the surgery was done badly. It most likely reflects the fact that the condition which caused the ganglion in the first place remains.
Patients can expect some discomfort from the incision for 4 - 6 weeks and discomfort from deep pressure for as long as several months. It is expected that a full recovery will be achieved within a few months after the surgery. Most people can return to their normal activities within 2-3 weeks of the surgery, although some people may restrict heavier activities for 4-6 weeks